The Importance of PPE in Preventing Healthcare-Associated Infections

A 2015 presentation from the Public Health Agency of Canada (PHAC) on the Canadian Nosocomial Infection Surveillance Program (CNISP) notes Healthcare-Associated Infections (HAIs) are a significant cost source, estimating CDI, MRSA, and surgical site infections alone account for more than CA$106 million in spending annually.
The World Health Organization (WHO) estimates HAIs are responsible for €7 billion in losses annually in Europe and US$6.5 billion in increased costs in the US.
The World Health Organization (WHO) estimates that HAIs are responsible for €7 billion in losses annually in Europe and US$6.5 billion in increased costs in the US.
No matter where global healthcare professionals are assisting patients, HAIs are a concern.
As such, many facets of managing HAIs are now built into the standard operating procedures and best practices of modern healthcare facilities — such as environmental sanitation, patient screening and triage, and proper use of antibiotics.
Huge portions of healthcare regulations and spending are also focused on the organizational and environmental facets of preventing and managing HAIs; however, there are two simple and effective methods for managing HAIs..
In this guide, we’re going to look at how effective hand hygiene protocols and proper PPE offer benefits for healthcare facilities of any size in the battle against HAIs.
What are Healthcare-Associated Infections (HAIs)?
Before we dive into how hand hygiene and PPE can help to prevent and reduce HAI incidents, it’s important to know a little about HAIs.
Also known as “nosocomial infections” or “hospital infections,” these infections are not present or incubating in patients at the time of admission. Symptoms may occur both during their stay or shortly after discharge.
Common HAIs include:
- Urinary Tract Infections (UTIs)
- Surgical site infections
- Gastroenteritis
- Meningitis
- Pneumonia
Common HAI Risk Factors

HAIs have a variety of transmission routes.
Contact transmission is one of the most frequent transmission routes. . It consists of both direct-contact transmission (transfer of the infection from a host to another person by direct physical contact) and indirect-contact transmission (contact with a contaminated intermedia object).
Droplet transmission routes, such as infection from sneezes or coughs, and airborne transmission routes, such as the airborne spread of Legionella, rubeola, or varicella viruses, are also concerns.
According to the WHO, common microbes responsible for HAIs include:
- Staphylococcus aureus (including MRSA)
- Streptococcus pyogenes (Group A Strep)
- Vancomycin-resistant Enterococcus (VRE)
- Klebsiella
- Enterobacter
- Pseudomonas
- Clostridium difficile (C. Diff)
- Candida
- Rotavirus
- Adenovirus
- Hepatitis A virus
- Norovirus
HAI risk factors are compounded by poor knowledge and application of basic infection control measures such as hand hygiene and proper use of PPE — including gloves, face masks and protective gowns.
Due to the prevalence of contact-based transmission, these sometimes overlooked foundational concepts are critical in the fight against HAIs.
Healthcare facilities that fail to recognize their importance, risk the health of their patients as well as their fiscal and regulatory health.
Simple Methods of Decreasing HAI Risk

As HAIs can happen anywhere within a healthcare facility, every worker plays a role in management and prevention.
From the admissions desk to the surgical floor, the following methods offer simple, cost-effective ways that healthcare professionals can minimize risk — both to themselves and their patients.
Hand Hygiene as a Component of Preventing HAIs
Hand cleaning is one of the most effective ways of preventing the contact-based spread of bacteria and viruses — but it’s also one of the most overlooked.
“While hand hygiene is not the only measure to counter HAI, compliance with it alone can dramatically enhance patient safety, because there is much scientific evidence showing that microbes causing HAI are most frequently spread between patients on the hands of health-care workers.” – World Health Organization
Hand cleaning often involves one of two methods:
- Soap and water
- Alcohol-based hand sanitizers
For soap and water cleaning, be sure to remove any items from your hands or wrists before washing. Use warm water and plenty of soap to ensure full coverage of your skin.
Lather and vigorously rub your hands together for at least 20 seconds, making sure you get not just your palms but the top of your hands, between your fingers, and up to — or even past — your wrists.
Rinse using plenty of clean water and dry thoroughly using an approved method.
Alcohol-based sanitizers are often used as a complementary system of hand cleaning as it requires less time and effort and kills most of the same microbes as soap and water washing. However, it is not always as effective.
Both methods can lead to drying skin and discomfort after endless shifts of handwashing. Not to mention, they do little to protect healthcare workers from the initial exposure to microbes and pathogens.
Using Single-Use Gloves to Supplement Hand Hygiene Routines

Single-use examination gloves are an excellent way to reinforce the benefits of hand cleaning routines, reduce the irritation and discomfort also caused by frequent hand cleaning, and provide an additional layer of protection between healthcare workers and patients.
When choosing the ideal glove for a situation there are several important considerations:
- Size: Gloves should offer a snug fit to minimize the impact on manual dexterity and reduce the chance of contaminants entering the glove cuff. However, they should not be so tight that they cause discomfort, increase the risk of breakage or tears, or become hard to remove.
- Protection Levels: Different risk levels and procedures will require different levels of coverage. For example, while standard gloves might be ideal for general interactions, other situations might require gloves with enhanced protection like extended cuff models.
- Material Choice: From patient or worker allergies to thickness and comfort, material choice can make a huge difference in the functional performance of a pair of disposable gloves. Be sure to consider the impact materials such as vinyl, latex, and nitrile will have before donning.
With a range of single-use glove types available, healthcare facilities can stay prepared for any situation while also ensuring optimal costs and performance across a broad spectrum of scenarios and requirements.
Care should also be taken to follow all donning, doffing, use, and disposal recommendations for gloves.
Contamination due to improper use, failure to change gloves as needed, or improper disposal could quickly negate any benefits offered and further increase risks to workers and patients alike.
You can find recommended uses, best practices, donning and doffing recommendations, and answers to common questions about exam gloves on our Examination Glove Standards & IFU page.
Medical Face Masks as a Means of Preventing Infection Spread

Medical face masks provide excellent control for infections spread through airborne particles or moisture droplets by covering the mucous membranes with filtering materials.
Face masks can protect healthcare workers who spend entire shifts surrounded by infectious microbes; however, their most effective use is as a barrier to prevent those who are already infected from spreading their condition.
As with all PPE, the design is also an important consideration because it will impact both functionality and comfort.
At the most basic level, when masks are more comfortable to wear, they are more likely to be worn and less likely to impact work performance.
Different mask designs and ratings will offer different levels of protection and overall effectiveness based on the microbes in question. As such, it is critical to match mask design to the intended function to ensure an optimal balance of protection, comfort, and cost.
Regardless of the mask chosen, proper donning, doffing, and disposal are essential to maximizing spread prevention potential. For more information on proper mask usage, consult our flu prevention guide and ASTM Mask Standards & IFU pages.
Medical Gowns, Head Covers, and Shoe Covers as a Means of Protecting Healthcare Workers and Avoiding Contamination
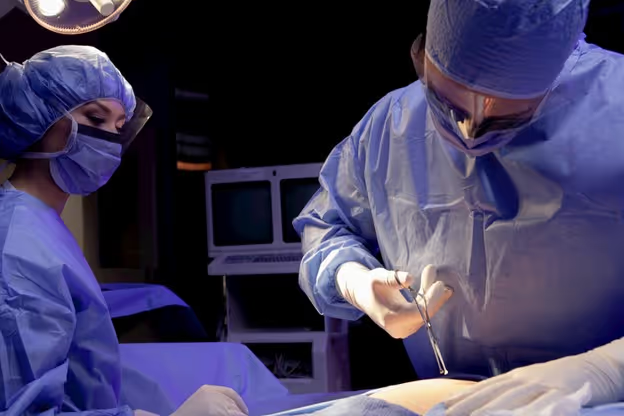
Medical gowns, head covers, and shoe covers all provide an effective means of controlling and preventing transmission of pathogens between environments or from non-sterile to sterile areas.
Critical design and performance considerations when choosing the proper items for infection control and prevention include:
- Liquid penetration resistance: By serving as an impermeable barrier, PPE with high liquid penetration resistance protects workers from exposure to blood and other bodily fluids.
- Bacterial filtration efficiency (BFE): PPE with high BFE ratings provides improved protection from exposure to airborne pathogens and contact-based transmission by reducing the ability for bacteria to reach the wearer.
- Weight: Heavy PPE can decrease comfort and impact the ability of healthcare professionals to perform their jobs. They can also make donning and doffing more difficult. When possible, keep PPE as light as possible while meeting protection requirements.
- Design: While design impacts protection coverage, it can also increase protection in other subtle ways. For example, easy-to-access ties and thumb loops can make gowns easier to don or doff and minimize gown shifting during procedures; while anti-slip tread on shoe covers can allow for safer movement across floor surfaces.
Material choice will ultimately have the biggest impact on the above considerations.
For example, SMS gowns offer far greater liquid penetration and BFE ratings than spunbond gowns of similar weight.
For more information on how material choices can impact gown performance, consult our SMS vs spunbond polypropylene guide.
Key Takeaways
- Person-to-person contact is a major risk factor for transmission and spread of HAIs
- When used together, hand washing and gloves help to offset downsides to both approaches and provide optimal benefits
- Gloves are not one-size-fits-all — materials, design, and sizing are critical
- Masks offer an effective, affordable barrier for infections which spread via airborne and moisture droplet transmission routes
- Gowns, head covers, and shoe covers can help to reduce the spread of infectious microbes between sterile and non-sterile areas while also providing an effective protective barrier for patients and healthcare workers
Simple steps — such as effective hand washing routines and proper use of disposable gloves — can greatly reduce HAI risks. PRIMED offers a wide range of PPE options to suit nearly any need. Our exclusive designs, wholly-owned supply chain, and in-depth understanding of modern healthcare protection needs positions PRIMED as a leading PPE provider in Canada. If you have questions about one of our products or how PPE can help your facility meet regulatory, safety, or compliance goals, contact us today or consult our clinical product information guides.
Related Resources
PRIMED Joins the Fight Against Bullying
February 25, 2026 is Pink Shirt Day. PRIMED proudly unites with hospitals across Canada to bring awareness to the movement that promotes kindness, inclusion, and respect.
%20400%20px%20Thmbnl.jpg)
PRIMED MRI Safe Mask: Safe by Design for Purpose-Built Protection
PRIMED's ASTM Level 3 MRI Safe Masks offer a high-quality, purpose-built solution that merges MRI compatibility with premium protection.

From the Sterile Core to the Decision Table: Elevating the Voice of MDR Professionals
MDR professionals don’t just process products, they influence how they are designed, selected, and standardized.
%20-%20Sterlization%20Wrap%20Display%20(1).jpg)

